Warfarin-Antibiotic Interaction Estimator
What exactly happens when these drugs interact?
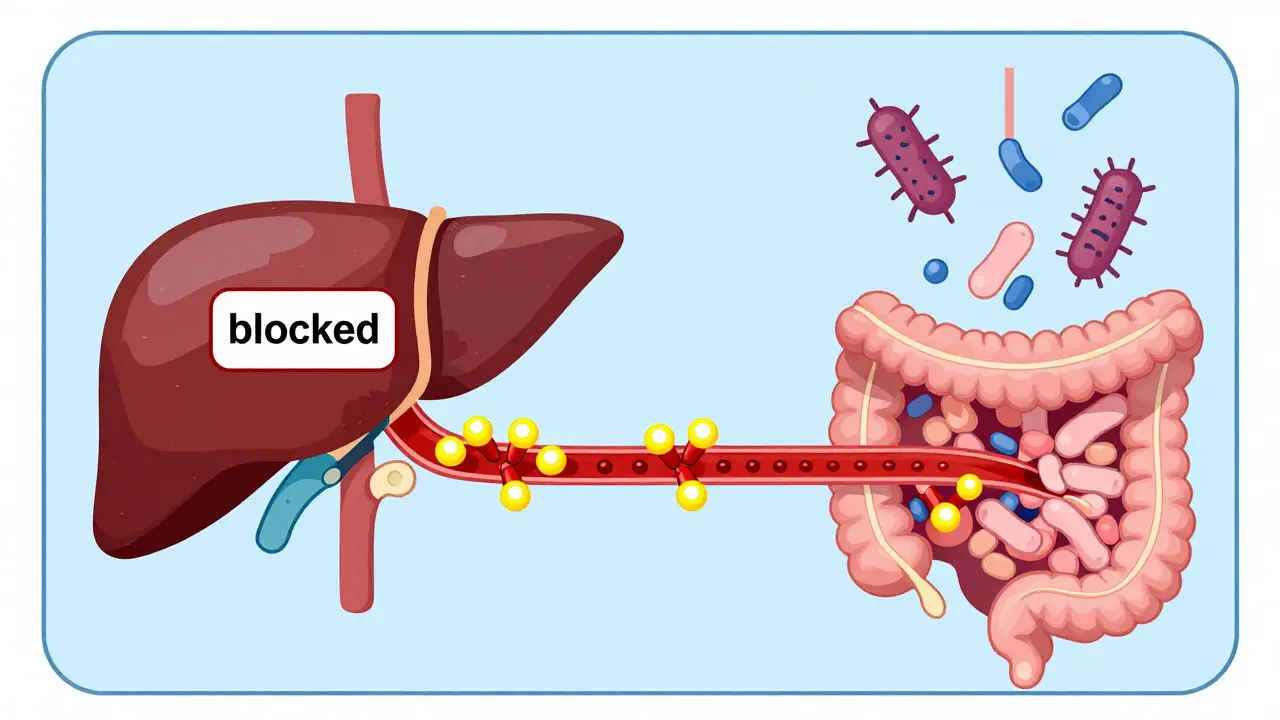
To understand the danger, we first have to look at how Warfarin works. This drug is a vitamin K antagonist that stops the body from recycling vitamin K, which is essential for creating clotting factors II, VII, IX, and X. Warfarin isn't just one molecule; it's a mix of two versions: R-warfarin and S-warfarin. The S-warfarin enantiomer is the real powerhouse, providing 60-70% of the anticoagulation effect and is about 3 to 5 times more potent than its counterpart. When you add Trimethoprim-Sulfamethoxazole (often called TMP-SMX or Bactrim) into the mix, three things happen simultaneously to push your INR higher:- Liver Enzyme Blockage: Trimethoprim acts as a moderate inhibitor of CYP2C9, the primary enzyme responsible for breaking down S-warfarin. When this enzyme is blocked, S-warfarin stays in your system longer, increasing its concentration by roughly 20-30%.
- Protein Displacement: Warfarin is incredibly "sticky," with 97-99% of it bound to albumin in the blood. Sulfamethoxazole competes for these same binding sites, kicking warfarin off the protein and leaving more "free" drug active in the bloodstream.
- Gut Flora Destruction: Like many antibiotics, TMP-SMX kills the bacteria in your gut that naturally produce vitamin K. Since warfarin works by opposing vitamin K, losing your internal supply makes the drug even more effective.
How fast does the INR spike?
This isn't an interaction that happens instantly, but it moves fast. Most patients see an INR elevation within 36 to 72 hours after taking their first dose of the antibiotic. Because it takes a few days to manifest, patients often feel fine initially, only to find their blood is dangerously thin by the time they return for a follow-up test. In real-world clinical settings, the jump can be staggering. While a typical therapeutic INR range might be 2.0 to 3.0, some patients have seen their levels rocket to 6.0 or even 8.0 within three days. This is especially common in elderly patients or those with mechanical heart valves, where the margin for error is slim.| Antibiotic Entity | Average INR Increase (Units) | Risk Level |
|---|---|---|
| Trimethoprim-Sulfamethoxazole | 1.8 (± 0.3) | High |
| Ciprofloxacin (Fluoroquinolone) | 0.9 (± 0.2) | Moderate |
| Amoxicillin | 0.4 (± 0.2) | Low |
Who is most at risk for a dangerous reaction?
Not everyone reacts the same way. Some people can take both medications with minimal change, but certain profiles are much more vulnerable. Data suggests that males are about 9% more likely to experience a significant INR spike than females. However, biological sensitivity plays a bigger role than gender. You are at a much higher risk if you fall into these categories:- Advanced Age: Patients over 75 typically show more volatile responses.
- Organ Impairment: Liver disease or decompensated congestive heart failure (CHF) impairs the body's ability to process both the antibiotic and the anticoagulant.
- Poor Nutrition: If you aren't eating enough vitamin K-rich foods (like leafy greens), you have no "buffer" to counteract the drug interaction.
How to manage the interaction safely
If a doctor decides that TMP-SMX is the only viable option-perhaps for a resistant UTI where Nitrofurantoin isn't appropriate-a strict monitoring protocol is mandatory. You cannot simply "wait and see." Medical guidelines recommend a three-step safety approach:- Baseline Check: Get an INR reading immediately before starting the antibiotic.
- The 48-Hour Window: Re-test the INR within 48 to 72 hours of the first dose. This catches the spike before it reaches critical levels.
- Preemptive Dose Adjustment: In high-risk patients, doctors often reduce the warfarin dose by 20-30% the moment the antibiotic is prescribed, rather than waiting for the INR to rise.
- INR 4.0 to 5.0 (No bleeding): Usually involves skipping one or two doses of warfarin and resuming at a lower level.
- INR > 5.0 (Minor bleeding): May require oral vitamin K (1-2.5 mg) to bring the levels down.
- INR > 10.0 (Severe bleeding): This is a critical emergency requiring IV vitamin K and Prothrombin Complex Concentrate (PCC) or fresh frozen plasma to replace clotting factors immediately.

The shift toward safer alternatives
Because this interaction is so volatile, many specialists now view TMP-SMX as almost contraindicated for patients on warfarin unless absolutely necessary. The rise of Direct Oral Anticoagulants (DOACs) has reduced the number of people on warfarin, but millions still rely on it, particularly those with mechanical heart valves who cannot use newer drugs. Education is the best defense. Research indicates that patients who receive specific counseling on how antibiotics affect their blood thinners have 37% fewer emergency room visits for bleeding. If you are prescribed a new medication, always ask: "Will this change how my blood thinner works?"Why does my INR go up when I take an antibiotic?
Antibiotics can increase INR by killing vitamin K-producing bacteria in the gut and by blocking liver enzymes (like CYP2C9) that normally break down blood thinners. This leaves more of the drug active in your system, making your blood thinner than intended.
Can I take Bactrim if I'm on Warfarin?
Yes, but only if your doctor determines it's the best drug for your infection and you agree to frequent INR monitoring. Due to the high risk of bleeding, alternatives like nitrofurantoin are often preferred for urinary tract infections.
What are the warning signs of an INR that is too high?
Watch for unusual bruising, nosebleeds that won't stop, blood in your urine or stool (which can look like coffee grounds or be dark red), and bleeding gums when brushing your teeth.
How often should I check my INR while on TMP-SMX?
You should have a baseline test, another test 48-72 hours after starting the antibiotic, and then every 3-4 days for the duration of the therapy to ensure your levels remain safe.
Does this interaction happen with all antibiotics?
No, but many do. TMP-SMX is among the highest risk. Others like ciprofloxacin have a moderate effect, while amoxicillin generally has a much lower impact on INR levels.