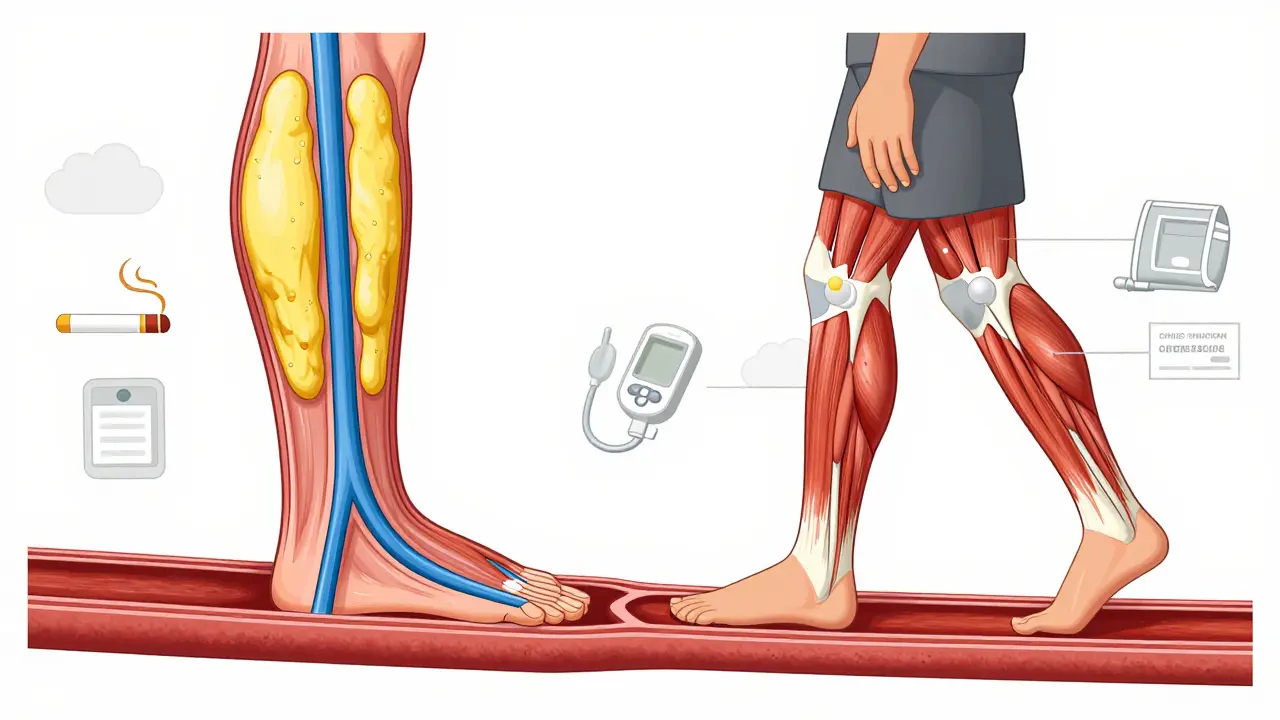
Peripheral artery disease, or PAD, isn’t just about leg pain. It’s a warning sign that your whole body’s blood vessels are clogging up. If you’re over 50 and smoke, or have diabetes, high blood pressure, or high cholesterol, you’re at risk-even if you don’t feel anything wrong yet. Many people brush off tired legs or slow healing sores as just part of aging. But those could be signs of something much more serious.
What Happens in Your Body With PAD?
PAD happens when fatty deposits build up in the arteries that carry blood to your legs, arms, stomach, or head. Most often, it’s the legs. This buildup, called plaque, slowly narrows the arteries. Less blood gets through. Your muscles don’t get enough oxygen, especially when you’re walking or climbing stairs. That’s when the pain starts.
It’s not just about discomfort. PAD is a red flag that you’re likely developing blockages in your heart or brain too. People with PAD have 3 to 5 times higher risk of having a heart attack or stroke than those without it. That’s why treating PAD isn’t just about helping you walk better-it’s about saving your life.
Common Symptoms You Can’t Ignore
The most classic sign is claudication. That’s when you feel cramping, aching, or tiredness in your calves, thighs, or buttocks while walking. It comes on during activity and goes away after a few minutes of rest. About 1 in 10 people with PAD have this symptom. The rest? They don’t feel anything at all.
But if you’re ignoring other clues, you’re putting yourself at risk. Look for:
- Cool or numb skin on your legs or feet
- Shiny, thin skin with less hair
- Toenails that grow slowly or become thick
- Sores on your toes, feet, or legs that won’t heal
- Pain in your legs even when you’re resting-especially at night
- Erectile dysfunction in men (yes, this is linked-up to 75% of men with PAD experience it)
These aren’t random aging changes. They’re signs your body isn’t getting enough blood. If you notice even one of these, especially if you’re over 50 or have diabetes, get checked.
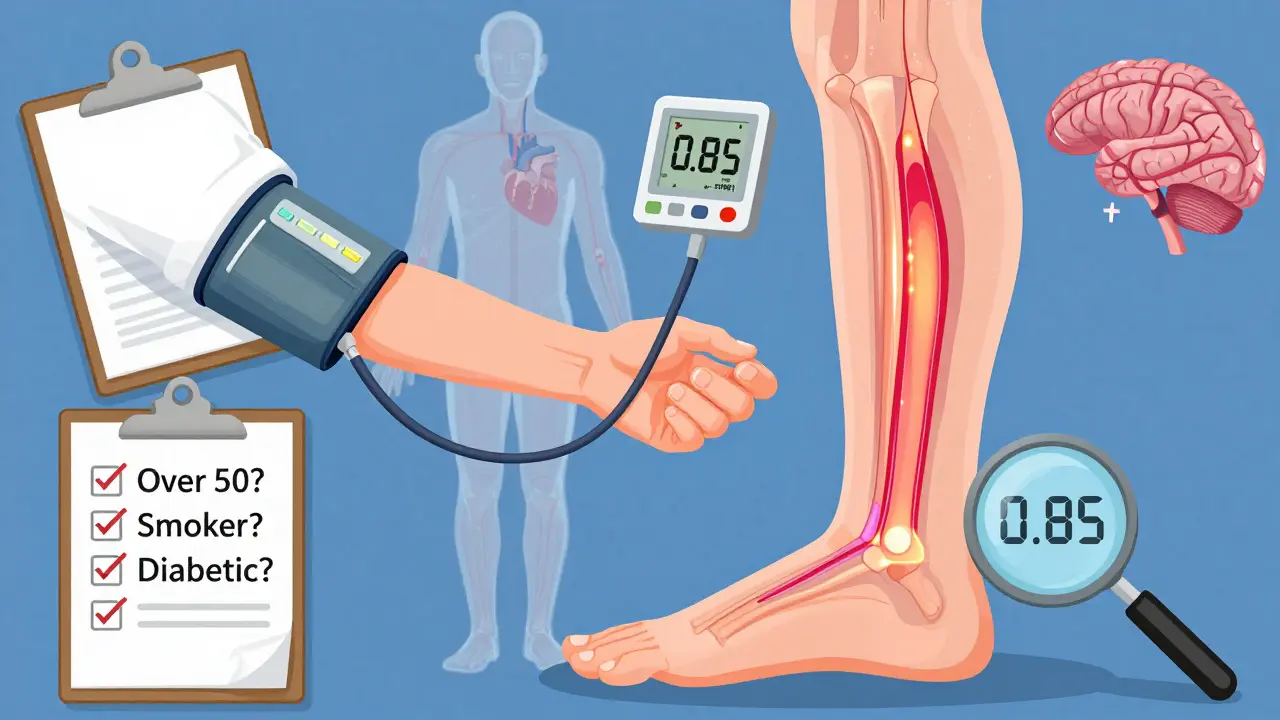
How Doctors Diagnose PAD
There’s no need for guesswork. A simple, painless test called the ankle-brachial index (ABI) can tell you if you have PAD. It compares the blood pressure in your ankle to the pressure in your arm. If the ankle number is 0.90 or lower, you have PAD. This test is accurate in 95% of cases.
For people with diabetes or kidney disease, the arteries can be stiff and hard to compress. In those cases, doctors use the toe-brachial index (TBI), which measures pressure in the big toe instead. A TBI under 0.70 means PAD is likely.
Other tests include:
- Doppler ultrasound-uses sound waves to see blood flow and spot blockages
- CT angiography-a detailed 3D scan that shows exactly where and how bad the blockage is
- MRI angiography-uses magnets and radio waves, no radiation
- Catheter angiography-the most accurate, but invasive. Used only if surgery is being considered
The American Heart Association recommends ABI screening for:
- Anyone 65 or older
- Anyone 50 or older with diabetes or a history of smoking
- Anyone 40 or older with multiple risk factors like high blood pressure, obesity, or family history
Yet, only 1 in 5 people who should be screened actually are. That’s a huge gap. Don’t wait for symptoms. If you’re in one of these groups, ask your doctor for the test.
How PAD Is Treated-Step by Step
Treatment isn’t one-size-fits-all. It starts with lifestyle changes, then adds medicine, and only if needed, moves to procedures.
1. Lifestyle Changes: The First Line of Defense
Quitting smoking is the single most important thing you can do. If you keep smoking, your risk of amputation goes up 8 times. Your chance of dying from heart disease triples.
Exercise is not optional-it’s medicine. A supervised walking program, done 3 to 5 times a week for 30 to 45 minutes, can improve your walking distance by 150% to 200% in just 12 weeks. You don’t need a gym. Walk until you feel pain, rest until it goes away, then walk again. Repeat. Over time, your body learns to use blood more efficiently.
2. Medications: Protecting Your Heart and Legs
Doctors usually prescribe three key drugs:
- Antiplatelets-like aspirin (81 mg daily) or clopidogrel (75 mg daily). These thin the blood slightly to prevent clots. Clopidogrel works better than aspirin for PAD patients, cutting heart attack and stroke risk by over 20%.
- Statins-like atorvastatin or rosuvastatin. They don’t just lower cholesterol. They stabilize plaque so it doesn’t rupture. All PAD patients should be on a statin, even if their cholesterol looks normal. They cut heart events by 25-30%.
- Cilostazol-a drug that opens up leg arteries and improves blood flow. It can double your walking distance, but it’s not safe if you have heart failure.
Controlling blood pressure and blood sugar (if you have diabetes) is just as important. High numbers speed up artery damage.
3. Procedures: When Medicine Isn’t Enough
If pain is keeping you from walking or your foot won’t heal, procedures may be needed.
- Balloon angioplasty-a tiny balloon is inflated inside the blocked artery to open it up. Works best for short blockages.
- Stent placement-a metal mesh tube holds the artery open after angioplasty. About 80% stay open after one year.
- Atherectomy-a device shaves off the plaque. Used when the blockage is hard and calcified.
- Bypass surgery-a vein from your leg or a synthetic tube is used to reroute blood around the blockage. Lasts 5+ years in most cases.
For critical cases-like a non-healing wound or gangrene-the WIfI classification system helps doctors decide urgency. Stage 4 means you have a 48% chance of losing your leg within a year if you don’t get treatment.
Why Early Detection Matters More Than You Think
PAD is silent until it’s not. By the time pain becomes severe, you may already have damage to your heart or brain. The 5-year death rate for people with PAD is 30-40%. That’s higher than many cancers. But if caught early, you can live a full life.
Studies show that people who quit smoking, exercise regularly, and take their meds reduce their risk of amputation by 70% and heart attack by 60%.
And here’s something most people don’t know: the U.S. passed the PAD Awareness Act in 2022. It’s now funding free screening programs for high-risk groups. If you’re eligible, ask your local clinic if they offer it.
What You Can Do Today
You don’t need to wait for symptoms. If you’re over 50 and smoke, or have diabetes, high blood pressure, or high cholesterol:
- Ask your doctor for an ABI test. It takes 10 minutes.
- Stop smoking-today. No delay.
- Start walking. Even 10 minutes a day. Build up slowly.
- Get your cholesterol and blood sugar checked. Know your numbers.
- Take your medications as prescribed. Don’t skip them.
PAD is treatable. But only if you act. Your legs-and your heart-are counting on it.
Can PAD be cured?
PAD can’t be completely cured, but it can be effectively managed. With lifestyle changes, medications, and proper care, you can stop the disease from getting worse, relieve symptoms, and prevent heart attacks, strokes, or amputations. Many people live full, active lives with PAD.
Is PAD the same as varicose veins?
No. Varicose veins are swollen surface veins caused by weak valves, and they’re mostly a cosmetic or comfort issue. PAD is a blockage in deeper arteries that reduces blood flow to muscles and tissues. The pain, healing problems, and risk of heart attack are unique to PAD.
Why do some people with PAD have no symptoms?
About 90% of people with PAD don’t feel classic leg pain. This is often because they’re less active, have nerve damage (like from diabetes), or their body adapts slowly. But even without symptoms, the artery blockage is still there-and still raising your risk of heart attack and stroke.
Can exercise make PAD worse?
No. In fact, exercise is one of the best treatments. Walking until pain appears, then resting, helps your body build new tiny blood vessels that bypass the blockage. Over time, you’ll walk farther with less pain. Avoiding exercise makes PAD worse.
What happens if PAD is left untreated?
Without treatment, PAD gets worse. Pain becomes constant, even at rest. Sores develop and won’t heal. Infection sets in. Without blood flow, tissue dies-leading to gangrene. In severe cases, amputation becomes necessary. Meanwhile, the same plaque that blocks leg arteries can rupture and cause a heart attack or stroke.
Is PAD more common in men or women?
PAD affects both men and women equally. But women are more likely to have atypical symptoms-like fatigue or weakness instead of classic leg cramps. This can lead to delays in diagnosis. Men are more likely to have erectile dysfunction as a sign, which is a strong clue.
How often should I get checked if I have PAD?
If you’ve been diagnosed with PAD, you should see your doctor at least once a year for blood pressure, cholesterol, and blood sugar checks. Your ABI should be retested every 1-2 years to track progress. If you’re on medication, more frequent visits may be needed to adjust doses or check for side effects.