When you pick up a prescription, you might see two options: the brand-name version you’ve heard of, or a cheaper generic. Many people wonder - does switching to a generic drug change how it interacts with other medications you’re taking? The short answer: no. The risk of drug interactions is essentially the same for generic and brand-name medications.
Why the confusion exists
It’s easy to assume generics are different. After all, they look different. They cost less. Sometimes, they come from a different manufacturer. And if you’ve ever switched from one pill to another and noticed a change in how you feel, it’s natural to blame the generic. But here’s the thing: the active ingredient - the part that actually treats your condition - is identical in both. The U.S. Food and Drug Administration (FDA) requires generic drugs to have the same active pharmaceutical ingredient (API), strength, dosage form, and route of administration as the brand-name version. That means if you’re taking a generic version of lisinopril, you’re getting the exact same molecule as the brand-name version, Zestril. The same goes for metformin, simvastatin, or sertraline. The chemistry doesn’t change. So why do people think interactions are different? The answer lies in what’s not the same: the inactive ingredients.What changes - and what doesn’t
Generic drugs can use different fillers, binders, dyes, or preservatives. These are called excipients. They help with manufacturing, stability, or how the pill dissolves. But they don’t treat your condition. Most of the time, they’re harmless. Lactose, cornstarch, and cellulose are common examples. But here’s where things get tricky. If you’re allergic to lactose, or have severe celiac disease, and your generic version uses lactose as a filler while the brand doesn’t, you might get a reaction. That’s not a drug interaction - it’s an allergy to an ingredient. It’s rare, but it happens. The FDA now lists excipients for all approved generics in its Orange Book, so pharmacists can check for potential issues. The real question is: do these differences affect how the drug behaves in your body? That’s where bioequivalence comes in.What bioequivalence really means
To get approved, a generic must prove it delivers the same amount of active drug into your bloodstream as the brand. The FDA requires this to happen within 80% to 125% of the brand’s performance. That’s a 45% range. Sounds wide, right? But in practice, most generics fall within 5% to 10% of the brand’s absorption rate. For most drugs, this tiny difference doesn’t matter. But for drugs with a narrow therapeutic index (NTI) - like warfarin, levothyroxine, or phenytoin - even small changes can matter. That’s why the FDA requires tighter standards for these: a 90% to 111% range. Pharmacists are trained to monitor these closely. A 2020 study in Scientific Reports looked at 17 cardiovascular drugs. It compared over 100,000 patients taking generics versus brand-name versions. The results? Generics were linked to lower rates of death and major heart events. That’s not a fluke. It’s likely because generics are cheaper, so patients take them more consistently.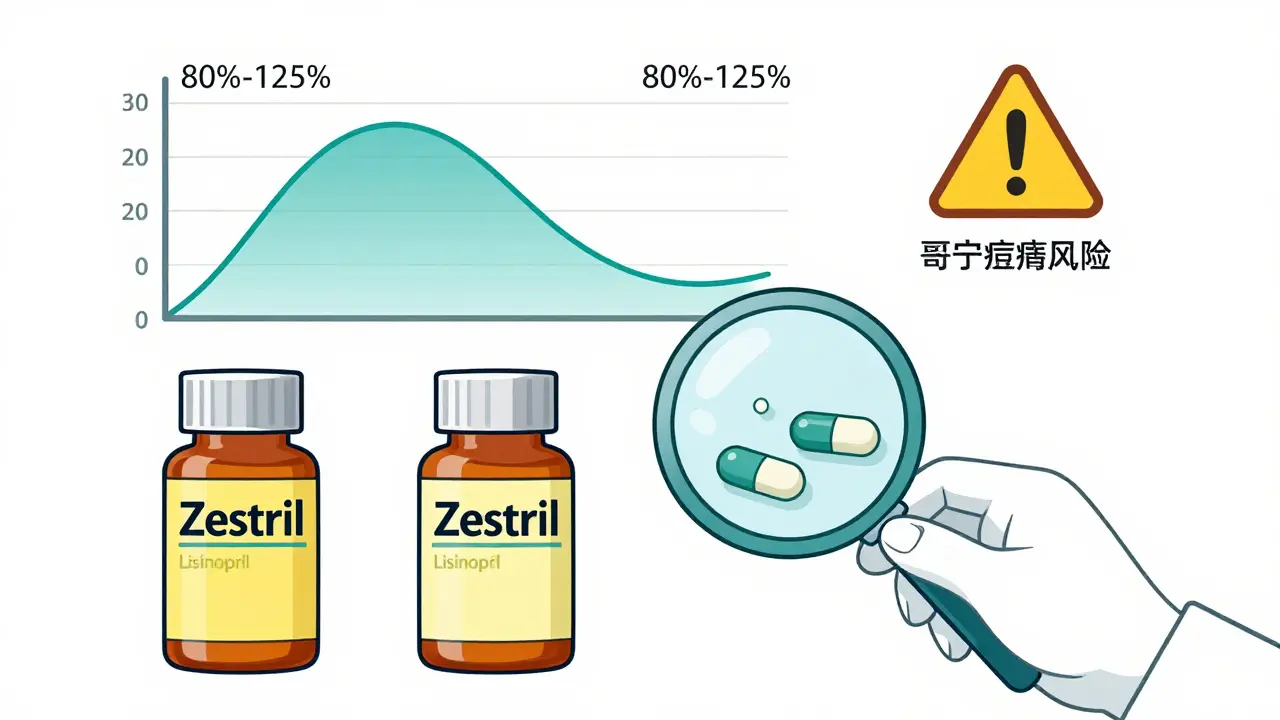
Do drug interactions differ?
Drug interactions happen because of how the active ingredient affects your liver enzymes, kidney function, or how other drugs are absorbed. Since the active ingredient is the same, the interaction profile is the same. Take warfarin, for example. It interacts with many antibiotics, supplements like vitamin K, and even grapefruit juice. Whether you’re on brand or generic warfarin, those interactions stay the same. The FDA’s Adverse Event Reporting System tracked over 100,000 reports from 2015 to 2020. The rate of interaction-related side effects was 0.78% for brand drugs and 0.82% for generics. That difference is statistically meaningless. Dr. Aaron Kesselheim from Harvard Medical School put it plainly: “The vast majority of evidence suggests that generic drugs are therapeutically equivalent to their brand-name counterparts, including regarding drug interaction profiles.”What about those stories online?
You’ve probably seen Reddit threads or Facebook groups where someone says, “I switched to generic and now I’m dizzy all the time.” Or, “My blood pressure spiked after the switch.” These anecdotes are real to the people who share them. But they’re not proof of a difference in interaction risk. Studies show that about 22% of people report changes after switching - but only 4% actually experienced a verified difference. The rest? It’s often the nocebo effect. If you believe the generic is inferior, your brain can make you feel worse. A 2022 Consumer Reports survey found that 18% of people thought generics had different interaction risks. But only 4% had personally noticed a change. That gap tells you everything.
What you should do
Here’s the practical advice:- If your doctor or pharmacist says the generic is safe, trust them. The science is solid.
- Keep taking your medication. Stopping because you’re worried about interactions is riskier than switching.
- If you notice new side effects after a switch, tell your provider. It might be the excipient, not the interaction.
- For NTI drugs like thyroid meds or seizure drugs, ask your pharmacist to stick with the same manufacturer if possible. Consistency matters more than brand vs. generic.
- Don’t assume brand-name drugs are safer. They’re not. They’re just more expensive.
What’s changing in 2026
The FDA is now tracking interactions between multiple generic versions of the same drug. Why? Because as more companies make the same generic, tiny formulation differences could pile up. A 2023 initiative called the “Generic Drug Shortage Prevention Program” is now monitoring how switching between manufacturers might affect patients. In Australia, where I live, the Therapeutic Goods Administration (TGA) uses the same standards as the FDA. Generic substitution is routine here. And the data? No spike in adverse events.Bottom line
Generic drugs aren’t “weaker” versions. They’re the same medicine, sold at a fraction of the cost. Drug interactions depend on the active ingredient. And that doesn’t change. Whether you’re on brand or generic, your body treats it the same way. The real risk isn’t in the pill you take. It’s in not taking it at all because you’re afraid of switching.Are generic drugs as effective as brand-name drugs in preventing interactions?
Yes. Generic drugs contain the same active ingredient as brand-name versions, so they interact with other medications, foods, and supplements in exactly the same way. The risk of drug interactions is not higher with generics. Regulatory agencies like the FDA and TGA require generics to prove bioequivalence, meaning they deliver the same amount of drug into your bloodstream as the brand.
Can inactive ingredients in generics cause drug interactions?
In rare cases, yes - but not in the way most people think. Inactive ingredients (like lactose, dyes, or preservatives) don’t directly alter how the drug interacts with other medications. However, they can cause allergic reactions or gastrointestinal upset in sensitive individuals. For example, someone with lactose intolerance might feel bloated after taking a generic that uses lactose as a filler. This isn’t a drug interaction - it’s an allergic or intolerance reaction. Pharmacists can check the excipient list in the FDA’s Orange Book to avoid these.
Why do some people say their symptoms changed after switching to a generic?
Many factors can explain this. The most common is the nocebo effect - when expecting a negative outcome leads to real physical symptoms. Studies show that when patients believe generics are inferior, they report more side effects. Other reasons include switching between different generic manufacturers (which can cause slight formulation differences), changes in dosage timing, or unrelated health changes. A 2022 Consumer Reports survey found that while 18% of people thought generics had different interaction risks, only 4% actually experienced a change after switching.
Are there any drugs where generics aren’t recommended?
For most drugs, generics are just as safe and effective. But for drugs with a narrow therapeutic index (NTI) - such as warfarin, levothyroxine, phenytoin, or cyclosporine - even small changes in blood levels can matter. While generics are still approved and safe, some doctors prefer patients to stick with one manufacturer to avoid potential variability between batches. This isn’t because generics are unsafe - it’s about consistency. Always talk to your pharmacist if you’re on an NTI drug and notice changes after a switch.
Can I switch back and forth between brand and generic without risk?
Yes, for most medications. The FDA approves generics to be interchangeable with brand-name drugs. Switching between them doesn’t increase interaction risk. However, if you’re on an NTI drug, frequent switching between different generic manufacturers could lead to small fluctuations in drug levels. For these cases, sticking with one version - whether brand or generic - is often recommended. Always inform your pharmacist if you’re switching between versions, so they can monitor for any changes.

Cory L
February 25, 2026 AT 05:42Also, if you’re blaming your generic for feeling weird, ask yourself: did you sleep? Are you stressed? Did you drink coffee at 10pm again? Maybe it’s not the pill. Maybe it’s your life.
Bhaskar Anand
February 26, 2026 AT 08:36William James
February 28, 2026 AT 02:58Also, if you’re scared of switching, talk to your pharmacist. They’re not just filling prescriptions-they’re keeping you alive. Trust them. They’ve seen this a thousand times.
David McKie
March 1, 2026 AT 08:18And don’t even get me started on the nocebo effect. You think people are just imagining it? Have you ever been on a drug that made you feel like garbage? Then switched and felt worse? You didn’t imagine it. You felt it. And now you’re being gaslit by a bunch of ‘science bros’ who think their degrees make them immune to human experience.
Southern Indiana Paleontology Institute
March 2, 2026 AT 01:40Anil bhardwaj
March 2, 2026 AT 21:35lela izzani
March 3, 2026 AT 07:37That said-yes, excipients matter. If you’re allergic to cornstarch or dye, check the label. I keep a printed list of excipients for common generics on my desk. It’s not hard. And if you’re on an NTI drug? I’ll call the manufacturer to confirm consistency. That’s my job. I’m not trying to sell you something. I’m trying to keep you safe. So if you’re worried? Talk to me. I’m here.
John Smith
March 5, 2026 AT 01:14