Managing blood sugar isn't just about picking the right pill or pen; it's about understanding the tightrope you walk between hyperglycemia and hypoglycemia. For millions of people, diabetes medications are life-saving, but they come with a set of rules that, if ignored, can lead to emergency room visits. Whether you're using a classic treatment like metformin or a modern injectable, the goal is the same: keep your glucose stable without letting your levels crash.
| Medication Class | Primary Safety Concern | Hypoglycemia Risk | Key Precaution |
|---|---|---|---|
| Metformin | Lactic Acidosis | Low | Check kidney function (eGFR) |
| Sulfonylureas | Severe Low Blood Sugar | High | Consistent carb intake |
| SGLT2 Inhibitors | Ketoacidosis (DKA) | Low | Stop before surgery |
| Insulins | Severe Hypoglycemia | Very High | Rotate injection sites |
The High Stakes of Hypoglycemia
The biggest worry for anyone on glucose-lowering therapy is hypoglycemia-when your blood sugar drops too low. It's not just a "shaky feeling"; it can lead to confusion, fainting, and in severe cases, coma. Sulfonylureas is a class of oral medications that stimulate the pancreas to release more insulin. These are notorious for causing crashes. In fact, research shows that 20% to 40% of people using these agents experience hypoglycemia, and about 1% to 7% hit a wall so hard they need someone else to step in and help them recover.
Then there is the "silent" danger: nocturnal hypoglycemia. About 30% of people with type 2 diabetes who are well-controlled on sulfonylureas experience blood sugar drops while they sleep without even knowing it. This is why continuous glucose monitoring (CGM) has become such a game-changer-it catches the dip before you wake up drenched in sweat or feeling exhausted for no apparent reason.
Insulin Safety and Administration
Insulin is the gold standard for type 1 diabetes and a necessary tool for many with type 2, but it requires precision. Insulin is a hormone used to lower blood glucose levels by allowing cells to absorb sugar from the bloodstream. The risk varies by type: rapid-acting versions like lispro hit quickly, while long-acting options like glargine provide a steady baseline.
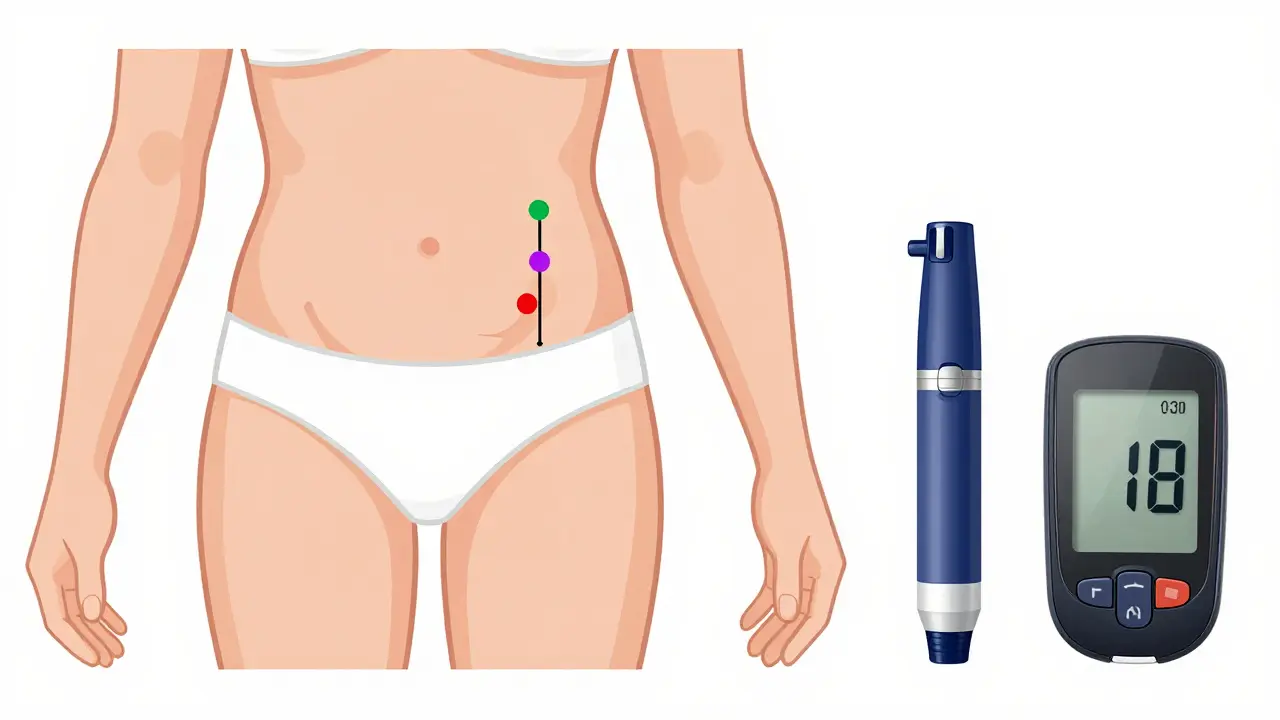
One of the most dangerous mistakes happens with concentrated formulations, such as Humulin R U-500. Because these are much stronger than standard insulin, a small dosing error can lead to a massive overdose. To stay safe, you must be obsessive about your injection technique. Rotating your sites-switching between the abdomen, thighs, and upper arms-prevents lipohypertrophy (hard lumps under the skin) which can make your insulin absorption unpredictable.
Navigating Oral Agents and Kidney Health
Not all oral meds work the same way, and your kidneys play a huge role in how they behave. Metformin is a biguanide medication that reduces glucose production in the liver and improves insulin sensitivity. While it rarely causes hypoglycemia, it can lead to a rare but deadly condition called lactic acidosis if your kidneys can't clear it from your system.
This is why doctors check your eGFR (estimated Glomerular Filtration Rate). If your eGFR drops below 30 mL/min/1.73m², metformin is generally off the table. If it's between 30 and 45, your doctor will likely lower the dose. If you have renal impairment but still need a sulfonylurea, glipizide is often the preferred choice because it's processed mostly by the liver, meaning it won't build up to toxic levels in your blood as easily as other drugs in that class.
The New Guard: SGLT2s and GLP-1s
Newer medications like SGLT2 inhibitors (which help the kidneys pee out excess sugar) and GLP-1 receptor agonists (which slow digestion and signal fullness) have changed the game for heart and kidney protection. However, they bring new risks. SGLT2 inhibitors can cause a specific, scary condition called euglycemic diabetic ketoacidosis (DKA). This is a state where your blood becomes acidic even though your blood sugar levels look relatively normal.
To prevent this, the AACE recommends stopping SGLT2 inhibitors immediately for emergency surgery and at least 24 hours before a planned procedure. You also need to be careful with extreme diets; very low-carb or ketogenic diets can actually increase the risk of DKA when combined with these meds. On the flip side, GLP-1 agents are famous for "stomach issues." Between 30% and 50% of users deal with nausea and vomiting, especially during the first few weeks of treatment.

Safety for Older Adults and Complex Care
Age changes how your body handles medication. For people over 65, the risk of falls increases dramatically. Dizziness and lightheadedness from a sudden blood sugar drop can lead to fractures or head injuries, which are far more dangerous in seniors than in younger adults. This is why "tight control" isn't always the best goal for an older patient; sometimes a slightly higher average blood sugar is safer than risking a severe crash.
Drug interactions also sneak up on people. For example, starting a course of antibiotics like sulfamethoxazole/trimethoprim can actually make your insulin work too well, causing an unexpected crash. Keeping a detailed medication log and using a Collaborative Drug Therapy Management (CDTM) approach-where your pharmacist and doctor work closely-can catch these conflicts before they happen.
What should I do if I feel dizzy while taking diabetes medication?
Dizziness is often a sign of hypoglycemia (low blood sugar). You should immediately check your glucose levels. If they are low, follow the 15-15 rule: consume 15 grams of fast-acting carbs (like 4oz of juice or glucose tabs), wait 15 minutes, and check again. If you are an older adult, sit or lie down immediately to prevent a fall.
Is it safe to use SGLT2 inhibitors before surgery?
No, it is generally not recommended. You should stop SGLT2 inhibitor therapy at least 24 hours before elective surgery to avoid the risk of diabetic ketoacidosis (DKA), a serious condition where the blood becomes too acidic.
Why does my doctor keep checking my eGFR for metformin?
Metformin is cleared from the body by the kidneys. If your eGFR (a measure of kidney function) is too low (typically below 30), the drug can build up in your system, increasing the risk of lactic acidosis, a life-threatening buildup of acid in the bloodstream.
What are the most common side effects of GLP-1 receptor agonists?
The most frequent side effects are gastrointestinal, including nausea and vomiting, which affect roughly 30% to 50% of patients. These usually occur when starting the medication or increasing the dose and often subside over time.
How do I prevent insulin injection site lumps?
The best way to prevent lipohypertrophy is by rotating your injection sites. Do not use the exact same spot every time; instead, move your injections across the abdomen, thighs, and arms in a systematic pattern to ensure the skin has time to heal.
Next Steps for Safe Management
If you're starting a new medication or feeling unstable, start by auditing your kit. Ensure you have a fast-acting glucose source always on hand and a reliable way to monitor your sugar. If you're over 65 or have kidney issues, ask your doctor for a specific "safety threshold"-the blood sugar level where you should stop worrying about the high and start worrying about the low.
For those struggling with dosing errors or frequent crashes, look into Automated Insulin Delivery (AID) systems. These "closed-loop" systems use algorithms to adjust insulin in real-time, significantly reducing the risk of nighttime lows and keeping you in your target range more consistently than manual injections.

